COVER STORY

Without Cornell's caring communiity, Kim, a 2010 Cornell graduate, says she might not be alive today.
Setting a trajectory for a life of health: Cornell's integrated approach to student well-being
Kim arrived at Cornell with the lifelong dream of becoming a doctor. At her Vancouver, British Columbia, high school, Kim – a 2010 graduate of the College of Human Ecology, who asked that her full name not be used – had excelled in class and beyond, showing talent in
gymnastics, volleyball and the arts, all while conducting research on adolescent health with faculty at a nearby university. As a Hunter R. Rawlings III Cornell Presidential Research Scholar, she soon saw that her classmates were just as talented.
"I realized how much more I needed to do to stand out in a place as academically incredible as Cornell," Kim says. A pre-med nutritional sciences major, she began to feel overwhelmed. While other students coped by socializing with friends or sweating at the gym, she worked harder at her research. She dropped sports and friends, and controlled the one thing she felt power over: how much she ate.
By the end of sophomore year, she had lost more than 20 pounds from her already-small frame, and her left foot became numb and weak. She went to Cornell's Gannett Health Services for evaluation and care. While Kim told herself that the symptoms had nothing to do with her weight, her health care providers urged her to get help related to her eating disorder. She resisted.
Kim studied harder and ate less. "I thought what I was doing was strong, motivated and directed toward success. But that was all in my head, because it was the absolute opposite. And of course the only person who didn't realize that was me," she says.
Concerned calls came from a wide range of faculty and staff members alarmed by Kim's frailty. This input provided additional leverage for Kim's doctor to insist on a meeting. She was so frail and malnourished that she could have suffered cardiac arrest at any time. "I knew I was busted. I couldn't fool myself any longer," she says. Kim's doctor told her she needed intensive inpatient care at an eating disorder treatment center. She broke down – and agreed to go.
"If it weren't for the people at Cornell who reached out to me from so many different places, I might not be alive today," says Kim, who not only recovered from her eating disorder but returned to Cornell to graduate and earned a master's degree in clinical nutrition from Columbia.
Kim is just one of a significant (and growing) number of Cornell students living with complex health conditions. Student health – for all students, not only those in crisis – is central to Cornell's mission: enabling students to reach their potential as scholars and citizens.
Cornell's approach is holistic and targeted, carefully tuned to the particular needs of this young-adult age group (see box, this page). From values expressed often by President David Skorton (who also is a professor in the departments of medicine and pediatrics at Weill Cornell Medical College) to prominence in the university's strategic plan and the living model of Cornell as a caring community, the university is a recognized national leader in campus health.
This comprehensive approach is evident at Gannett, where a multidisciplinary health team serves students. Stories like Kim's also underscore the difference it makes – to students in need and those concerned about them – to be part of a larger community that has a core commitment to health and well-being. This commitment is evident across the campus: in advising offices and residence halls, in programs like the Cornell Healthy Eating Program and Let's Talk, through student groups like EARS (Empathy, Assistance and Referral Service) and Cornell Minds Matter and in the university's participation in broad student health initiatives like the National Collaborative for Hazing Research and Prevention.
Care for the student body … and mind
"As a university president, physician and parent, I know how important good health is to the achievement of both immediate and lifelong goals," Skorton said. "We can all be proud that [Gannett] is a national model for integrating the delivery of physical, mental and public health services, and that thoughtful and compassionate efforts are underway across the Cornell campus to promote the health and well-being of our community, especially of our students."

Dr. Janet Corson-Rikert, right, executive director of Gannett Health Services, with Gregory Eells, director of Gannett's Counseling and Psychological Services (CAPS).
Dr. Janet Corson-Rikert, executive director of Gannett and associate vice president for campus health, agrees. "Cornell makes an enormous investment in recruiting students and offering them a wonderful, diverse educational community with an incredible array of courses and research opportunities with world-class faculty," she says. "But medical research has shown that brains don't learn optimally without physical and emotional health. You don't maximize learning and achievement without maintaining the health of the body and the brain."
The impact of Cornell's educational investment is measured over the long term – across a graduate's lifetime, she says, "so interventions that foster lifelong patterns of health and self-care are critical components of Cornell's educational value."
Gannett distinguishes itself as a university health service in its integrated delivery of medical and mental health services. Multidisciplinary teams (doctors, nurses, counselors, therapists, educators and others) work together to coordinate care for illnesses and injuries, provide preventive services, and enhance students' abilities to maximize their health. During medical visits, students are routinely screened for depression, anxiety and high-risk alcohol use. A student who comes in for a sinus infection but also may be struggling with depression will receive care for his sinuses and a personal referral to appropriate counseling support.
In 2012, Gannett was one of the first college health centers in the country to be recognized as a Patient Centered Medical Home. Widely accepted as the model for how primary care should be organized and delivered throughout the health care system, the PCMH designation is awarded to primary care organizations that are patient-centered, comprehensive, team-based, coordinated, accessible and focused on quality and safety.
The impetus for Cornell's approach to campus health came with the arrival of Corson-Rikert in 1995 from Phillips Exeter Academy, where she had served as director of health services. As a pediatrician with an adolescent medicine specialization, she found enormous opportunity in being able to practice medicine within a residential community. At Exeter, she worked closely with mental health counselors to provide integrated care for students whose health concerns often intertwined medical, social and emotional components. She also worked with faculty and administrators to develop institutional policies and systems that leveraged the caring and expertise of faculty and staff to mitigate risks and augment support for students.
"When I arrived at Cornell," Corson-Rikert says, "I recognized the challenge of applying similar principles and approaches to a student body of 20,000. Fortunately, my colleagues here joined me in embracing the challenge."
Each year, more than 80 percent of students come to Gannett for health care; 28 percent utilize Gannett's Counseling and Psychological Services (CAPS) before they graduate. Most of the health problems Cornell students identify as impediments to academic performance are related to mental health, from stress and relationship difficulties to anxiety and depression.
Since 1996, the number of visits to Gannett for CAPS has nearly tripled (see chart, p. 10). "This is not necessarily an indication that college is more stressful than ever," says Gregory Eells, director of CAPS. More students come to universities with a history of mental health challenges than in the past, thanks to more effective treatments, as well as destigmatization of these issues. Students also may be more willing to seek help when they need it.
"Sometimes they need some encouragement or help dealing with the complexity of their situations, which is why we educate the entire campus about how to recognize and respond to students in need," says Timothy Marchell '82, Gannett's director of mental health initiatives. Marchell and his colleagues have developed innovative bystander intervention programs that cultivate a widespread network of "eyes and ears" – members of the Cornell community who can recognize students in need, consult with health care and student service providers, and connect students to helpful resources. More than half of all Cornell faculty members and nearly all key staff members have been trained in Cornell's "Notice & Respond: Assisting Students in Distress" program.
A campus commitment

Kaitlin Hardy '12 with her gymnastics coaches, Melanie Dilliplane and Paul Beckwith. See larger image
As a sophomore, Kaitlin Hardy '12 had an epileptic seizure in her chemistry lab and lost consciousness. Her doctors from home changed her epilepsy medication, but it made her foggy and sleepless. She couldn't keep food down, was too weak to walk to class and eventually was hospitalized for dehydration. "I was just in really rough shape," she says.
Hardy was a member of the gymnastics team; an athletic trainer noticed her difficulties and asked her to consider taking a health leave of absence from Cornell. Athletics staff helped her talk with her coaches, and Student Disability Services staff coordinated a plan with faculty members to make up academic work.

Matt Simmonds '14 See larger image
Hardy returned to campus the following spring with Gannett assistance in coordinating her support team. "I went from thinking that I was in this alone, and it was my own battle to fight, by myself and for myself, to knowing I had people behind me every step of the way in case I should fall," she says. By senior year, she had gone to Gannett so often the staff knew her student number. "They weren't just concerned with giving me fluids and making sure I was physically OK and sending me out the door," Hardy says. "They cared about me as a whole person."

Matt Simmonds '14 on the field. See larger image
Now a master's degree candidate in epileptology (neurology that specializes in epilepsy treatment) at King's College, London, Hardy has applied the lessons she learned at Cornell by seeking out such accommodations as extra time to take exams because her medication can affect cognitive function.
Similarly, health services, academic and athletics staff worked together to help Matt Simmonds '14 recover from three football-related surgeries within 10 months. A professor extended deadlines for a course and offered tutoring while Simmonds also consulted with an academic adviser. Meanwhile, head football athletic trainer Bernie DePalma kept Simmonds positive through two physical therapy sessions every day.
Without that support, "in my mind, there is no way I would still be here," Simmonds says. "My body wouldn't be where it is today, and without the academic help, I would be doing a lot worse."
Enhancing the learning environment
"For all the students who receive help, we know others are out there struggling on their own," says Catherine Thrasher-Carroll, mental health promotion coordinator for Gannett.
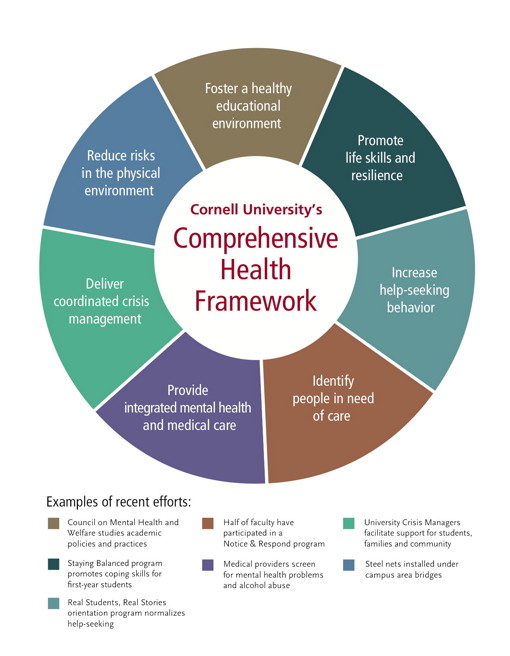
Cornell's comprehensive health framework graphic.
In the 2008 National College Health Assessment, nearly 40 percent of students reported that they were unable to function at least once during the past year due to depression. Similarly, in a 2013 Cornell survey (PULSE: Perceptions of Undergraduate Life and Student Experiences), nearly 40 percent of undergraduates said that they had been unable to function academically for at least a week during the past year because of stress, depression or anxiety (the survey was completed by 6,190 undergraduates, a 45 percent response rate).
"These data underscore not only the need for a broad safety net of caring individuals, but also the need to move further upstream and help individuals cope with the challenges inherent in college life," Thrasher-Carroll says. "My position was created to support this effort."
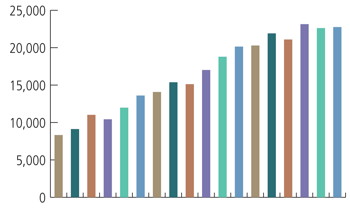
Since 1996, the number of visits to Gannett for counseling and psychological services has nearly tripled. See larger image
Gannett staff members are part of a growing movement within the field of public health. Its goals are not only preventing foreseeable health risks and managing chronic health concerns, but also helping individuals and communities maximize their capacity for health and well-being. When applied to a student community, this focus directly supports the link between health and academic performance. "You wouldn't recruit an athlete to come here and then not give them equipment, training and practice," says Marchell, himself a former Cornell athlete. "Similarly, we need to support students' health so that they can achieve their academic potential."
Recent research confirms that students need resilience and emotional health to learn, says Janis Whitlock, Ph.D. '03, a research scientist in the Bronfenbrenner Center for Translational Research. The term "resilience," which refers broadly to one's ability to recover quickly from disappointment or setback, unpacks into many elements, many of which affect academic and cognitive performance. "For example," Whitlock notes, "studies show that simply experiencing positive emotion, even if subtle or experimentally induced, not only enhances a person's ability to approach problems in novel ways, but also their focus, curiosity and willingness to entertain new ideas and connections. And it can enhance memory storage and retrieval."
Gannett staff members collaborate with students, staff and faculty on a wide array of initiatives that teach skills and attitudes to foster resilience in the face of life's inevitable vicissitudes, Whitlock says; this is based on emerging science showing that the skills needed to enhance well-being can be learned. "There is increasing evidence that resilience is malleable and can be fostered through practices such as stress and time management, mindful meditation and cognitive exercises that focus on optimism and gratitude," she says.
A comprehensive approach

Catherine Thrasher-Carroll, mental health promotion coordinator for Gannett Health Services during a WSKG community conversation. See larger image
The combination of integrated clinical services, education for the community and strategies to foster a supportive environment together constitute a comprehensive approach to student health and well-being. This approach is designed to tackle complex community health issues (e.g., alcohol abuse, sexual violence, hazing, suicide prevention, infectious disease) that affect individuals within the context of their living-learning communities (see diagram, this page).
This model informed Cornell's multifaceted response following a cluster of suicides on campus in 2009-10, including the collaboration with the city of Ithaca to install steel nets under the bridges that span Ithaca's iconic gorges (see story, p. 8).
"We aim to engage the entire Cornell campus in supporting student health and well-being," says Susan Murphy '73, Ph.D. '94, vice president for student and academic services. "Every semester the concerted efforts of faculty, staff and students themselves help us create a caring community."
Life lessons

Timothy Marchell '82, director of mental health initiatives for Gannett. See larger image
For some students, challenging times and a proactive health care system not only support academic success, but also shape academic interests. The medical and psychological support Kim got at Cornell translates directly to her work today.
Now a senior research coordinator in gastroenterology at Johns Hopkins University, Kim is considering getting a doctorate – but only if that path makes her happy. "My dream since I was a kid didn't really change, but I learned a better way to go after it," she says. "I learned that through the things that Gannett did for me, the things that faculty did for me, and so many people within HumEc. I owe them so much."
"We are moved by the tenacity and spirit of our students every day," says Corson-Rikert. "And, because every student's journey to and through Cornell is unique, it's both a challenge and a privilege to provide essential services to help them set a trajectory for a life of health and well-being."
Resources
Gannett Health Services
Cornell's 'Caring Community'
www.news.cornell.edu/categories/campus-life/caring-community
Gannett's 'Notice & Respond'
www.gannett.cornell.edu/notice